What to expect from your newborn...
Unfortunately, babies don’t read the baby books you have read and come without an instruction manual. And to make things worse, they have a ‘no returns’ policy! The following can/will happen to small babies and are normal:
‘My baby is very sleepy in the first 24-48 hours’
This is normal. Being born is hard work! If your baby sleeps for more than 4 hours without feeding, or develops a low blood sugar level, the nursing staff will assist by either expressing breast milk and feeding it to your baby, giving a supplementary feed or calling your paediatrician. When to worry? If you are persistently unable to wake your baby for feeds once you have been discharged from hospital.
‘My baby wants to feed all the time’
This is called cluster feeding and typically happens on the second night after birth. It is guaranteed to drive most moms to tears and even have them considering leaving their babies at the hospital upon discharge. This is a normal part of the initiation of breastfeeding. This is your baby’s way of stimulating breast milk sufficiently to meet demand. In this time many moms give in to the temptation of giving supplementary formula feeds. This is then actually detrimental to the supply of breast milk and should be discouraged.
‘My baby vomits occasionally’
Babies often swallow amniotic fluid and blood during the birthing process. This causes them to vomit occasionally in the first 24-48 hours after birth. The vomit may even be blood stained. This is either from blood swallowed during the birth process, or sometimes from cracked and bleeding nipples in the breastfeeding mom. When to worry? If the vomiting is persistent and severe or dark green in colour and if your baby fails to pass the first stool within 24 hours of birth.
‘My baby has a skin rash’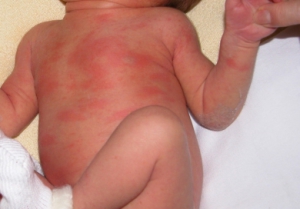
New borns develop many skin rashes that are harmless and resolve spontaneously without treatment. The most common is a rash with the terrible name, ‘Erythema toxicum’. This red skin rash can develop from the 2nd day and consists of red spots, often with a yellow pustule in the centre. It can be wide spread, occurring on the face, limbs, body and the diaper area. When to worry? If your baby is also lethargic, unable to feed or having a fever.
‘My baby seems to be passing blood in the urine’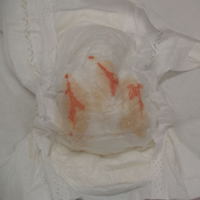
In the first few days/weeks of life, the urine of a baby often seems to be blood tinged. This is because of a mineral that is deposited in the urine and is normal. Babies may also pass urine very infrequently in the first week of life. Only after a week will the baby be having 6-8 wet nappies per day.
‘My baby girl has a vaginal discharge’
Baby girls develop a vaginal discharge from the withdrawal of maternal hormones. This can even be bloody. It is normal and resolves spontaneously.
‘My baby’s breasts are swollen’
This is also because of the effect of maternal hormones. It can cause swelling of one or both breasts. This will resolve spontaneously after a few weeks. When to worry? If the swelling is red, warm and painful and/or your baby is febrile or not feeding well.
‘My baby has a blocked nose’
Most babies have a blocked nose for the first weeks/months of life. This often sounds as if it is coming ‘from the back of the nose’ and causes the baby to make a snorting sound when crying or feeding. This is a harmless, albeit very frustrating condition. For symptomatic relief, one can use a salt water containing nasal spray frequently. Suctioning devices seem to make very little difference and humidifiers will probably make it worse. When to worry? If your baby has a runny (as opposed to blocked) nose, coughing, is febrile and unable to feed.
‘My baby has a bump on the skull’
This is called a cephalohaematoma or scalp bleed. It is seen more frequently after normal vaginal deliveries, but can also be seen after a caesarean section. This is because of bleeding into one of the layers of the scalp. It resolves spontaneously, but may take weeks or months to do so. It may even become quite hard as organization of the blood happens. When to worry? If the swelling is extensive and your baby is pale and/or jaundiced and unwilling to feed.
‘My baby has a yellow colour’
Many babies will develop jaundice. Mild jaundice in an alert baby that is feeding well, doesn’t need treatment. It is, however, notoriously difficult to judge how yellow a baby is just by looking at the skin. If there is a concern about jaundice, your paediatrician could request a test to check the level of bilirubin. The treatment for jaundice could be done in the hospital or at home. Be sure to alert your paediatrician if the mom has a negative blood group, or if a previous baby needed treatment for jaundice.
Fever
Fever is one of the most common reasons for visits to our practice. It is also one of the most feared conditions that is sure to cause panic in any parent. Once you understand a few simple things about fever, it is not so scary anymore:
- Fever is defined as a temperature of 37.6 C and higher
- It is only a symptom. This is the body’s mechanism to fight an infection.
- During the time of acute illness, fever will spike every few hours, regardless of what you do. Fever will always be higher at night.
- There is no set value for a ‘dangerous fever’. A child could be gravely ill with even a low grade fever.
- A young baby (less than 3 months of age) always needs to be seen urgently if they have a fever.
- Danger signs in a child with fever are: Inability to feed, inability to wake your child, difficulty in breathing or convulsions. If your child is alert and playful in-between the spikes of fever, he is unlikely to be in danger.
- Fever can be treated at home with oral or rectal Paracetamol or Ibuprofen.
- If the fever lasts for more than 3 days, or if there are danger signs, it is advisable to have your child checked out.
Blocked nose and/or coughing
This is also a very common reason for consultations. This is something that is particularly common in the creche going child.
- A child with a cold has a runny/blocked nose and sneezing, with/without fever, with/without coughing.
- A child with a cold only needs symptomatic treatment like a nasal spray, a safe cough syrup and pain and fever management. Make sure your child takes enough fluid. Stay clear of over the counter cold and flu preparations and cough syrups. The symptoms normally last for 5-7 days.
- A child with flu has a sudden onset of very high fever and feeling unwell. There could be headache, nausea & vomiting, abdominal pain and sometimes respiratory symptoms as well. This is more serious than a cold, and is mostly preventable by yearly flu vaccination.
- Influenza also needs the symptomatic treatment mentioned above, but in some cases an antiviral medication needs to be prescribed.
Vomiting and/or diarrhoea
This is another favourite ailment of the creche going child. The most common reason is a viral gastroenteritis. The child will typically have vomiting and diarrhoea with/without fever that lasts for 3-5 days. The most important part of the treatment is oral rehydration to prevent dehydration. This needs to be given in small, frequent volumes to prevent vomiting. Medical attention should be sought if the fever lasts for more than 3 days, the diarrhoea lasts for more than 5 days or there is blood or slime in the stools. Admission may be needed if your child refuses oral fluids, or continues to vomit even clear fluids.
